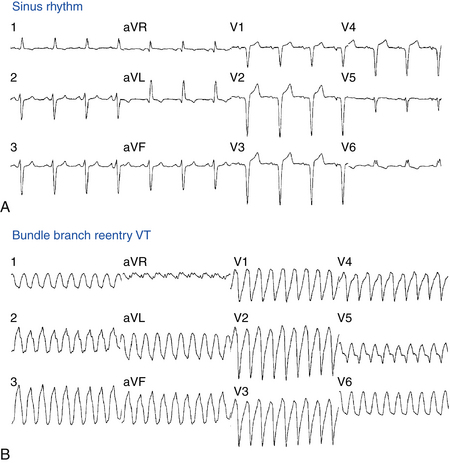
Whether the diagnosis is SVT (atria driving the ventricles) or VT (ventricles driving the atria) cannot be determined with a 1:1 AV relationship. About 30% of VTs conduct retrogradely to the atria, and have a 1:1 VA relationship. Inability to find P-waves, or finding a 1:1 association between QRSs and P-waves is not helpful as both SVT and VT can produce this.This proves that atria are not needed for the mechanism of the arrhythmia. A variation of this includes AV association but finding more QRSs than P-waves (see example).AV dissociation proves that atria and ventricles are independently activated.Highly favours VT (Spec 98%, Sens 82%), but only seen in 20-50% of VTs (Brugada et al 1992).There are two main tools to distinguish VT from SVT with aberrancy: P-waves (AV dissociation) and QRS morphology – “how likely is it that this is an SVT with a bundle branch block?”.Significant proof is needed to dissuade you towards SVT. A useful approach is to start with a presumed diagnosis of VT, which will be correct 80-90% of the time.We recommend you become familiar with the Brugada criteria, since it is well known and frequently tested on exams. All of these algorithms are derived from the core principles, which we teach here. (Brugada criteria, Vereckei algorithm, Lead II criteria, etc.). There are numerous scoring systems and algorithms developed to distinguish these two entities.The best tool is to look at the baseline ECG for evidence of pre-excitation. Pre-excitation (pre-excited SVT) is quite rare.Artifact can also be ruled out, as it often produces non-physiologic signals on ECG, often in a single lead.Pacing is easily ruled out with clinical history, physical exam, and absence of pacing spikes.Other differential diagnoses are often easily excluded: Two most important differential diagnoses of WCT are VT and SVT with aberrancy.NOTE: Some VT rhythms are adenosine sensitive, particularly outflow tract idiopathic VT.No response to 24mg of adenosine generally means the tachycardia is insensitive to adenosine, and does not require the AV node in its mechanism (VT). 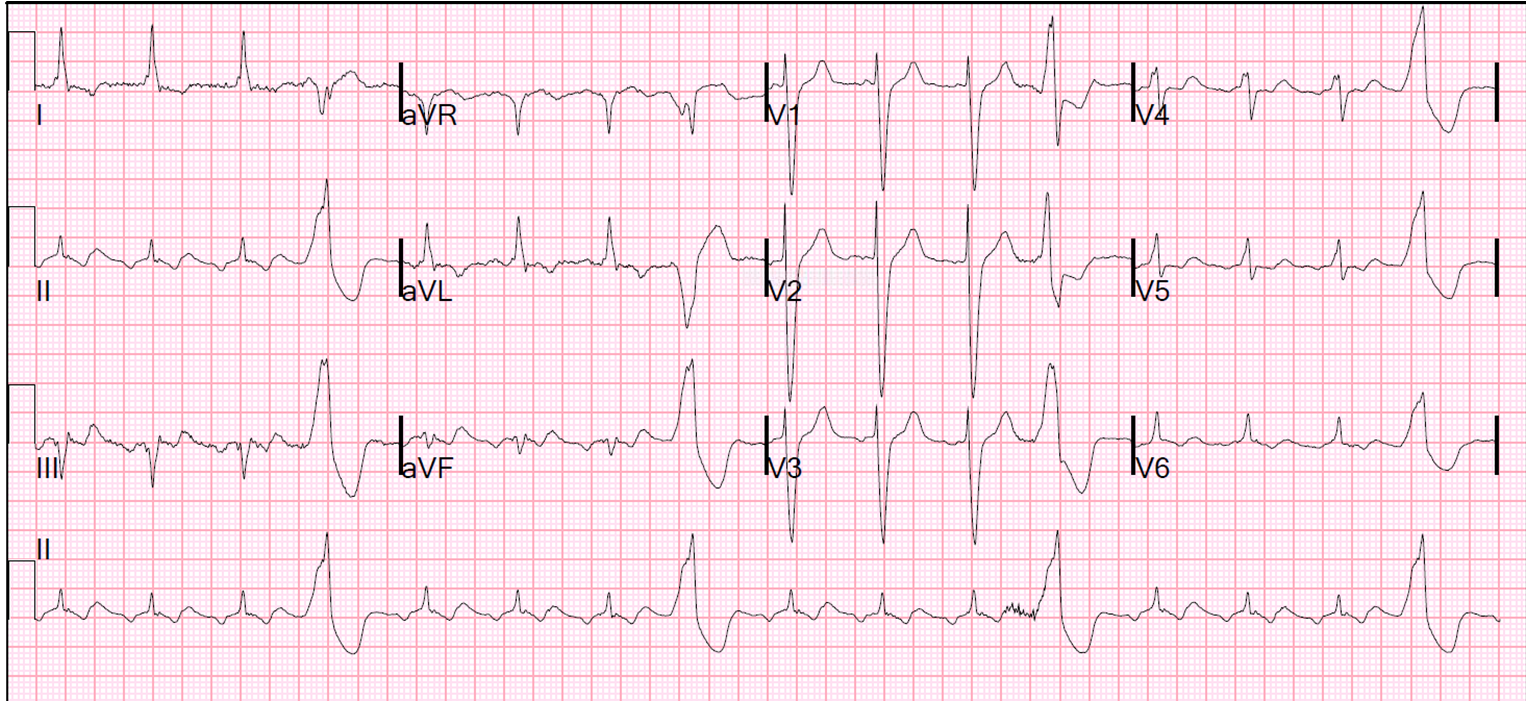
With each injection warn the patient about the sensation of adenosine, and check to ensure the IV line is functional.If no effect, then can be doubled to 24mg IV. If no effect, dose is doubled to 12mg IV. Start with 6mg adenosine IV followed by rapid IV saline flush.Adenosine generally has no effect on VT.Adenosine will result in a transient AV block, which may terminate some re-entrant SVTs, or block conduction to the ventricles to reveal atrial activity (such as atrial tachycardia).Very helpful diagnostically to distinguish VT from SVT.Vagal maneuvers – can produce transient AV block, which can terminate some re-entrant SVTs.Only should be done for hemodynamically unstable patients with crash cart ready to deliver cardioversion if necessary.Anomalous Aortic Origin of a Coronary Artery.Non-Bacterial Thrombotic Endocarditis (NBTE).Acute Coronary Syndrome: ACE Inhibitors, Beta Blockers, MRAs.Driving Guidelines for Arrhythmia/Syncope.Cardiac Implantable Devices for Residents.2014 CCS Thoracic Aortic Disease Guideline Summary.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
